What Is a Dental Crown? Types, Procedure, Cost & Benefits
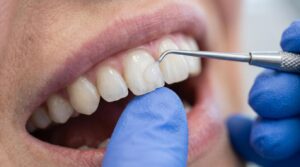
A dental crown is a tooth-shaped cap that covers and protects a damaged or weak tooth. Dentists use crowns to fix the tooth’s shape, size, strength, and look. Crowns are also used on dental implants and teeth that have had root canal treatment. They can be made from porcelain, metal, or resin based on your needs. With good care, dental crowns can last for many years. People hear the word crown and immediately think about cost or pain. It is not just a cap. It is a way to save a tooth that would otherwise be lost, and to restore your ability to chew, speak, and smile without pain or embarrassment. At Vista Dorada Dental, we walk every patient through this process so nothing comes as a surprise. What Is a Dental Crown? A dental crown is a custom-made cap that fits over a damaged or decayed tooth. It covers the entire visible part of the tooth above the gumline and restores its appearance. Once it is cemented in place, it works just like a natural tooth and handles the full pressure of chewing and biting. Dentists recommend crowns when a tooth is too damaged for a filling but still worth saving. This includes cracked teeth, teeth with large old fillings, teeth that have had a root canal, and teeth that have worn down significantly over time. A crown protects what is left of the natural tooth and gives it a second chance to function properly for many more years. When Do You Need a Dental Crown? A dental crown may be needed when a tooth is damaged, weak, cracked, worn down, or treated with a root canal and needs extra protection. Broken or Cracked Teeth A cracked tooth can be painful and unpredictable. Some cracks are small enough to be managed without a crown, but when a crack runs deep or causes pain when you bite down, a crown holds the pieces together and prevents the crack from spreading further into the root. Large Fillings That Weaken Teeth Every time a cavity is filled, some natural tooth structure is removed. When a tooth has a very large filling, especially one that takes up most of the tooth, the remaining walls become thin and fragile. A crown covers the entire tooth and prevents those thin walls from fracturing under pressure. After Root Canal Treatment A root canal removes the infected pulp from inside the tooth. This process saves the tooth but also leaves it more brittle because the tooth loses its internal blood supply. Most back teeth that have had a root canal need a crown placed over them immediately after to prevent fracturing during chewing. Worn-Down Teeth Teeth grinding, also called bruxism, and acid erosion from diet or acid reflux can wear teeth down significantly over time. When a tooth becomes too short or flat to function properly, a crown rebuilds it to the correct height and shape so your bite works the way it should. Cosmetic Improvements Crowns are sometimes used to improve the appearance of a tooth that is severely discolored, misshapen, or poorly proportioned. While veneers are often the first choice for cosmetic work, a crown is a better option when the tooth also has structural damage that needs addressing at the same time. Types of Dental Crowns Dental crowns come in different materials, including porcelain, metal, ceramic, and resin, each offering different benefits for strength, appearance, and durability. Porcelain Crowns Porcelain crowns are made entirely from ceramic material and closely match the natural color and translucency of real teeth. They are the most aesthetic option available and are a popular choice for front teeth where appearance matters most. The downside is that they are slightly less durable than metal-based options and can chip under heavy biting force. Ceramic Crowns Ceramic crowns, including those made from zirconia, have become the most widely recommended option in modern dentistry. Zirconia is extremely strong, tooth-colored, and biocompatible, meaning it does not irritate the gums. It works well for both front and back teeth and is now the most commonly placed crown type in most dental offices. Metal Crowns Metal crowns, including gold and other alloys, are the most durable option available. They rarely chip or break and require very little tooth structure to be removed during preparation. The only real downside is their appearance. Most patients use metal crowns on the back molars where they are not visible. Porcelain-Fused-to-Metal Crowns These crowns have a metal base covered with a porcelain outer layer. They offer a balance between strength and aesthetics and were the most common crown type for many years. However, the metal base can sometimes show a dark line at the gumline as the gums recede, and the porcelain layer can chip over time. Resin Crowns Composite resin crowns are the most affordable option. They look natural but wear down faster than porcelain or metal options and are more prone to fractures. They are sometimes used as a cost-effective solution but are generally considered a shorter-term option. Dental Crown Procedure Step by Step Learn what happens during a dental crown procedure, from the first examination and tooth preparation to placing and fitting the final crown. Initial Dental Examination Before any treatment begins, your dentist will examine the tooth thoroughly and take X-rays to assess how much damage is present, whether the roots and surrounding bone are healthy, and whether a crown is the right treatment. If the tooth has significant decay or infection, that needs to be addressed first. Tooth Preparation On the day of the procedure, the tooth is numbed with local anesthesia. The dentist then reshapes the tooth by removing a thin layer from all sides to create room for the crown to fit over it. If the tooth is severely broken down, the dentist may need to build it up with filling material first so there is enough structure to support the crown. Taking Impressions or Digital Scans Once the tooth is prepared, an